Introduction:
Kawasaki disease (KD) and its coronary sequelae impose substantial economic burden in all societies. IVIG access is heterogeneous in MENA region, with common out-of-pocket expenses. KD management costs required this first multinational cost-of-illness (COI) evaluation conducted within KAWARABI, the Kawasaki Disease Arab Initiative in MENA-region.
Methods:
This COI study used a decision-tree model reflecting real-world KD management over a 2-year horizon from a societal perspective. Data were collected via structured questionnaire completed by 17 clinical sites from 14 MENA countries, supplemented with national publicly available databases.
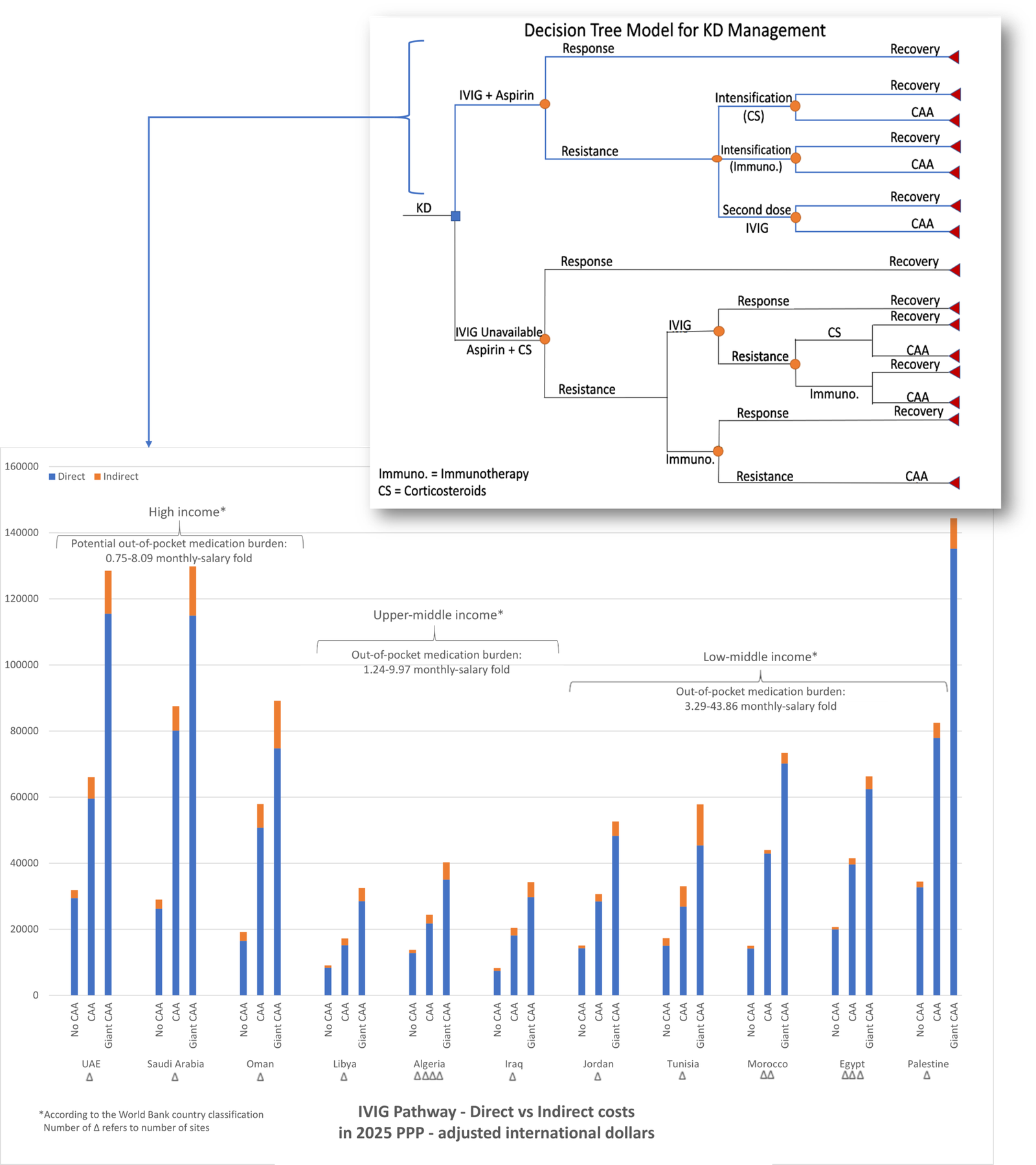
Two management pathways were modeled (Figure-top): an IVIG-available pathway (with escalation options, or second-dose IVIG in refractory cases) and an IVIG-unavailable pathway (aspirin-corticosteroids, with delayed IVIG or biologic escalation); Model outcomes included recovery or development of coronary artery aneurysms complications (CAA). Direct medical costs (hospitalization, medications, imaging, laboratory, follow-up visits, and professional fees) and indirect costs (caregiver productivity loss and transportation) were estimated. Costs were assessed for uncomplicated disease and for CAA. Cross-country comparative costs used 2025 purchasing power parity (PPP)-adjusted international dollars.
Results:
Uncomplicated IVIG-available pathways, per-patient total costs ranged from $14,964 to $34,442 in low-middle income countries, $8,288 to $13,758 in upper-middle income countries, and $19,163 to $31,849 in high-income countries. Treatment escalation increased mean costs by 41% with corticosteroid intensification, 54% with biologics, and 69% with a second IVIG dose. CAA increased mean costs by up to 120% and giant CAA by up to 271%. In uncomplicated IVIG-unavailable scenarios, costs ranged from $19,320 to $48,857 in low-middle settings, $7,582 to $10,424 in upper-middle income settings, and $19,836 to $34,691 in high-income settings. Major cost drivers were IVIG (40-60%), hospital length-of-stay (11% if recovery, 16–18% with escalation strategies), biologic therapies (14%), and imaging/exams (5-9%). Indirect costs contributed up to 22.95% (increased disproportionately in complicated cases) (Figure-bottom). Out-of-pocket medication costs equated to 0.75-43.86 months of salary.
Conclusion:
KD represents a major economic burden, amplified by treatment resistance and coronary complications. In addition to improving patient outcomes, early diagnosis and optimized treatment access alleviates prohibitive preventable expenses. A forthcoming cost‑effectiveness analysis will integrate clinical outcomes to guide service planning and funding decisions.